The Sacrum And Respiration
At the 2005 annual IOA conference – Sequencing: the Art of Finding the Key, Kenneth Klack, D.O. posed a question concerning the Mitchell pelvic axis system and its effect on the respiratory diaphragm. I am going to do my best to respond to that question here.
The Mitchell pelvic axis system was proposed by Fred Mitchell, Sr. D.O. as a way to explain the motion of the sacrum around the innominates. The system defines six axes around which the sacrum and innominates move. The axes are described using surface landmarks. They are as follows:
1) The anterior/posterior axis through the center of S2.
2) The middle transverse axis, which lies at the level of the PSIS and is the axis, which sacral flexion and extension dysfunctions occur. Some schools refer to these as the unilateral shears.
3) The superior transverse axis, which lays one finger width above the PSIS and is the axis about which the cranial rhythm (primary respiration) is predominantly focused.
4) The inferior transverse axis, which lays one finger width below the PSIS and is where innominate rotation primarily occurs. Innominate rotational dysfunctions occur on this axis.
5) The left oblique axis appears when the middle transverse axis shifts up on the left and down on the right. This occurs when the sacrum side-bends to the right e.g. during the walking cycle. Sacral torsions occurring on the left axis (ex. left on left) happen here.
6) The right oblique axis appears when the middle transverse axis shifts up on the right and down on the left. This occurs when the sacrum side-bends to the left e.g. during the walking cycle. Sacral torsions occurring on the right axis (ex. left on right) happen here.
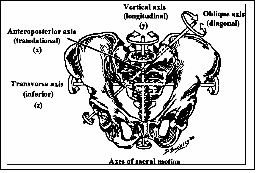
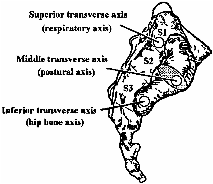
Pictures from the Glossary of Osteopathic Terminology
To answer the question I began by consulting Paul Hume, N.D, and D.O. from New Zealand who was also at the course. Paul and I started with “working” sacrum’s that had no perceptible dysfunctions and proposed the following test – we would restrict the axes one at a time and observe what happened to the body. To restrict the axis the patient is held around that axis to restrict motion – e.g. to restrict motion around the middle transverse axis the patient would be held with circumferential compressive force between the ASIS and PSIS. To restrict the superior transverse axis, circumferential force is applied between the ASIS and one finger width above the PSIS, etc.
Prior to the test, the patient was asked to take a deep breath and note the sensation of breathing. Once the operator’s hands were positioned, a compressive force was applied circumferentially to the innominates and the patient was asked to take a deep breath and compare that with the original breath.
The observations were:
a) Pressure on the middle transverse did not effect respiration. Patients reported no change in breathing.
b) Pressure on the superior transverse gave a sensation of a weight or heaviness in the sternal area and the patient felt like they were taking a less deep breath.
c) Pressure on the inferior transverse axis gave a sensation of weight of heaviness in the area of the respiratory diaphragm and the patient felt like they were taking a lees deep breath.
d) Pressure on the left oblique axis gave a sensation of left sided breathing restriction with no effect on the right.
e) Pressure on the right oblique axis gave a sensation of right sided breathing restriction with no effect on the left.
f) The A/P axis was not tested.
While a dedicated scientific approach, such as the use of spirometry, may give more highly specific data, the N of 10 used in the answering of this question seems to indicate a likely correlation between the Mitchell axis system and diaphragmatic respiration. Participant responses to the perception of restricted breathing were similar throughout the process. Because of this experiment, I have been looking with new eyes at all of the pelvic dysfunctions that I treat. I am noticing more subtle changes in rib cage and diaphragmatic motion and correlating it with the pelvis. I am asking my patients to experience their breathing more, both before and after treatment. It is making me a better osteopath. Thank you Kenneth.
